The Diabetes-Wound Connection: Managing Risks for Better Health
Diabetes, a chronic condition affecting millions worldwide, has far-reaching impacts on overall health, including a significant influence on wound healing. Understanding the diabetes-wound connection is crucial for effective management and prevention of complications. By exploring this vital aspect of diabetes care, we can empower individuals to take proactive steps towards healthier, complication-free lives.
The Physiology of Wound Healing
The human body has a remarkable capacity to heal itself, and the wound-healing process is a prime example of this inherent ability. Under normal circumstances, wound healing involves a complex series of actions coordinated among various types of cells and tissues. Initially, the body works to stop the bleeding through the clotting cascade and then moves on to the inflammatory phase where white blood cells clear out infection and debris. Following this, new tissue forms in the proliferative phase, and finally, the wound is remodeled and strengthened over time.
For individuals with diabetes, this finely tuned process is often derailed. Elevated blood glucose levels have a domino effect on the body's healing mechanisms. They can impact the function of white blood cells, reduce the production of growth factors that aid in repair, and even modify the structural components of the skin. The impaired blood flow often associated with diabetes can inhibit the delivery of essential oxygen and nutrients to the wound site, and neuropathy, another complication of diabetes, can decrease sensation, leading to delayed detection and treatment of injuries.
Diabetes-Related Wounds: A Closer Look
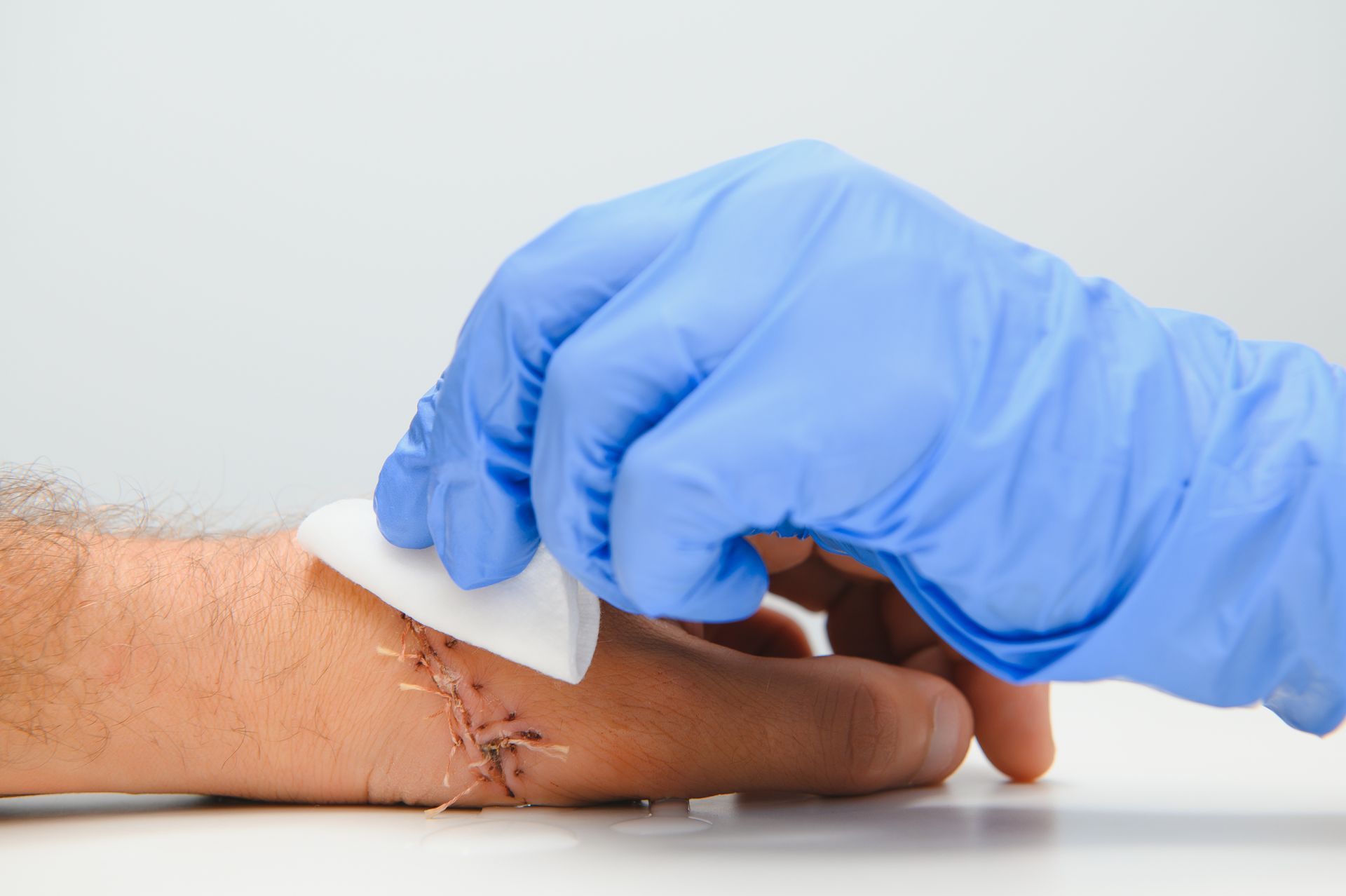
Diabetic patients are particularly prone to certain types of wounds, notably diabetic foot ulcers. These ulcers are often the result of a combination of factors, including neuropathy, poor circulation, and altered biomechanics of the foot due to diabetes. Apart from foot ulcers, people with diabetes may also be at risk for non-healing wounds resulting from surgical incisions, infections, or trauma that may not resolve readily due to their compromised healing capacity.
In Salt Lake County, including the Murray area, these challenges are well-recognized by healthcare providers. While exact
statistics on diabetic wounds at the local level may vary, the national data reflects a considerable burden on individuals and healthcare systems alike.
Prevention: The First Line of Defense
Maintaining controlled blood sugar levels is paramount in reducing the risk of wound development and poor healing outcomes. A consistent management plan for diabetes, including medication, diet, and exercise, is the foundation of prevention. Regular inspections of the feet for any injuries or changes are crucial, as compromised sensation may not always signal an issue. Identifying concerns early can lead to timely interventions.
Equally important to regular monitoring is wearing suitable footwear designed to reduce pressure points and friction that could lead to ulcers. Such preventive measures, along with a balanced diet rich in nutrients that support skin integrity and physical activity to improve circulation, lay the groundwork for minimizing wound-related complications in diabetic patients.
Early Detection and Management
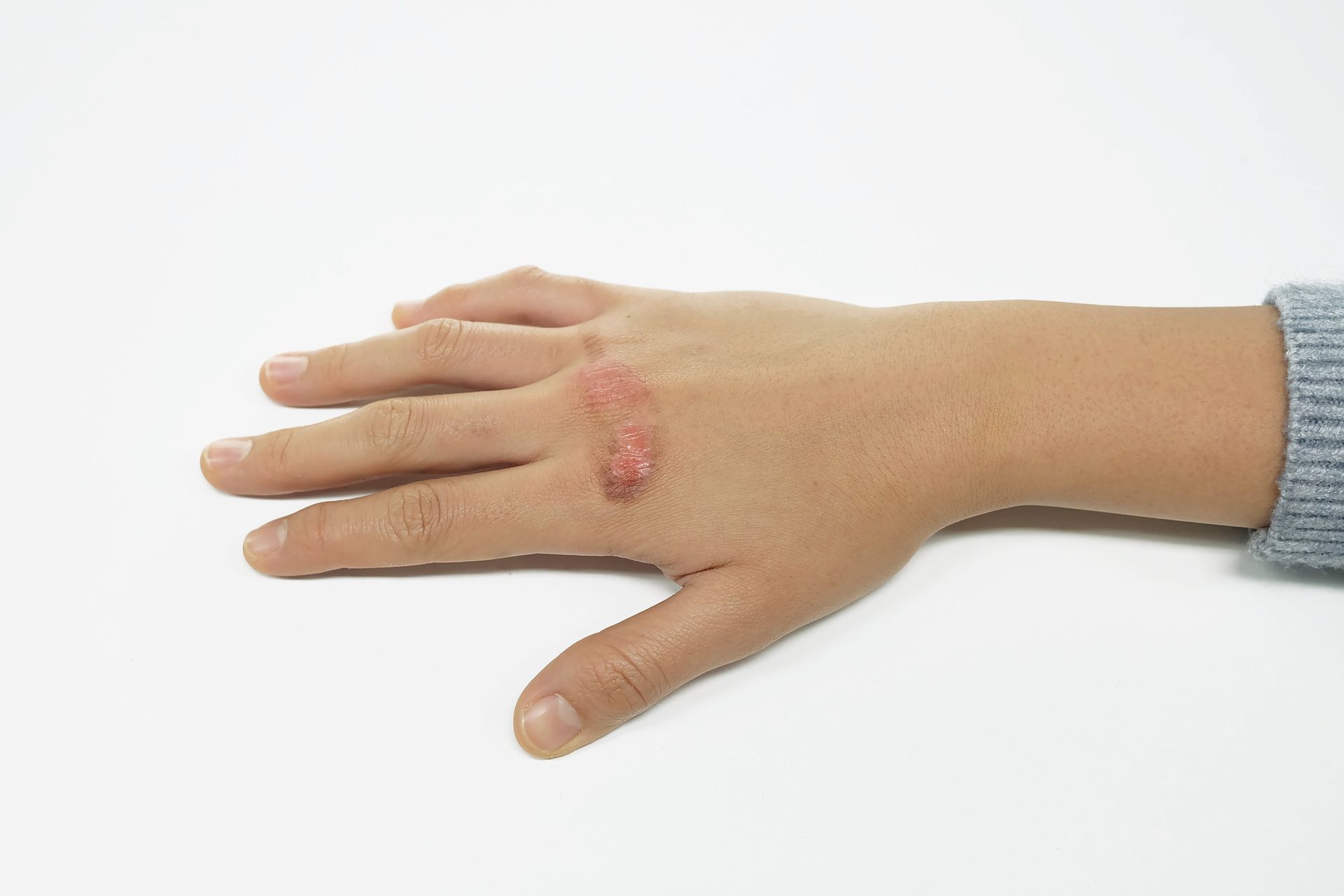
Recognizing the signs of wound infection, such as redness, warmth, swelling, or discharge, is essential for individuals with diabetes. These symptoms, along with any new pain in the affected area, should prompt a visit to a healthcare provider. Swift attention not only has the potential to halt the progress of an infection but also opens the door to a comprehensive approach to care.
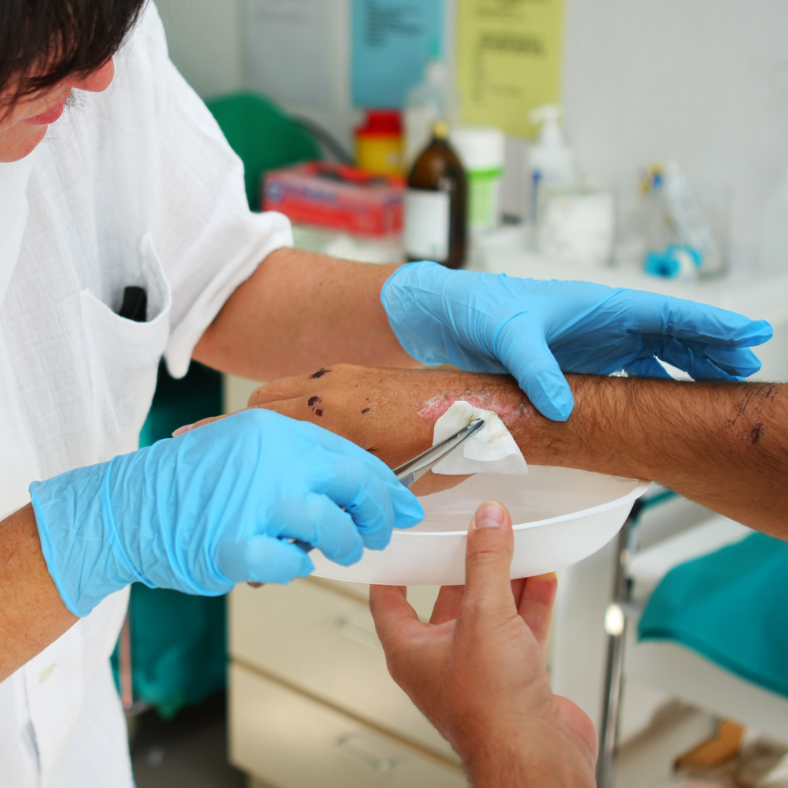
In the context of chronic wound management, interdisciplinary care involving specialists in endocrinology, podiatry, wound care, and sometimes vascular surgery becomes integral. This team approach caters to the multifaceted needs of the patient, addressing the wound itself while also managing underlying conditions that may impede healing. Patient education becomes a key counterpart to clinical interventions, empowering individuals to take an active role in the prevention of serious complications.
Advanced Wound Care Techniques
The landscape of wound care has substantially grown with the advent of advanced treatments. Innovation in wound care technology has led to new developments that significantly enhance the healing process. For instance, methods such as negative pressure wound therapy and hyperbaric oxygen therapy have emerged as a boon to those struggling with non-healing wounds related to diabetes. These treatments work by promoting the formation of granulation tissue or enhancing oxygen delivery to the wound, respectively.
The rising importance of
regenerative medicine in wound care cannot be overstated. The use of bioengineered tissues and growth factor therapies has started to alter the healing paradigm, offering hope for faster recovery and better outcomes. While these more sophisticated therapies may seem futuristic, they are increasingly becoming integrated into standard care, especially for wounds that display a protracted healing trajectory.
As such technologies evolve, healthcare providers in Murray, Utah, and beyond continue to monitor and adopt practices that show promise in facilitating better wound healing for diabetic individuals.
Living with Diabetes in Murray, UT: Community Resources
Living with diabetes can be challenging, especially when facing the risk of chronic wounds. Murray, UT, offers a supportive network for those in need. Local healthcare facilities have programs tailored to the unique needs of diabetic patients, including outpatient wound care centers that specialize in treating chronic wounds.
Community support groups and events provide platforms for education and emotional support, allowing individuals to share experiences, tips, and encouragement. These resources can be invaluable for patients who need continuous engagement and support to manage their condition effectively. Similarly, staying abreast of benefits, such as nutrition counseling and foot care services, is critical to preventing wounds and promoting overall health.
Regular check-ups with healthcare providers, including specialists in endocrinology and podiatry, are essential for the early detection of complications and to ensure that the management plan is up-to-date and responsive to an individual's evolving needs.
Patient Stories and Testimonials
An important aspect of understanding the gravity of diabetes-related wounds is listening to the stories of those who have faced these challenges. Anonymized patient testimonials from the Murray area and broader Salt Lake County showcase the resilience and courage of individuals managing their wounds. These narratives often highlight not only the clinical challenges but also the psychological impact that a successful wound-healing journey can have on a person's life.
The emotional toll of living with a non-healing wound is substantial, affecting the quality of life, self-esteem, and daily activities. Stories of recovery and improved health can serve as powerful testimonies to the effectiveness of comprehensive wound care and can inspire others to seek timely and specialized treatment.
The Importance of Personalized Care Plans
Each patient's journey with diabetes and wound care is unique, and personalization of care plans is critical for effective treatment. Personalized care involves tailoring wound care strategies to address each individual's specific medical, nutritional, and lifestyle needs. This approach might include custom-wound dressings, specialized footwear to offload pressure, or specific dietary modifications to support wound healing and overall health.
The interplay between good wound care and nutrition is a significant focus. A diet rich in proteins, vitamins, and minerals is vital for repair and can make an appreciable difference in healing rates. For patients in Murray, UT, and the wider region, understanding the relationship between diet and wound healing is an often overlooked aspect of diabetes management that healthcare providers aim to emphasize.
The Role of Health Insurance and Affordability
Understanding health insurance coverage is a critical component of managing diabetic wound care. Coverage for procedures, specialized treatments, and outpatient services can vary widely among insurance plans. It's important for those living in Murray, UT, to work closely with their healthcare providers to navigate these complexities. Providers can help clarify which treatments are covered under a person's plan and also offer assistance with prior authorizations or alternative solutions when necessary.
Healthcare affordability remains a significant concern for many, especially for those dealing with chronic conditions like diabetes. Hence, it becomes vital to open a dialogue with wound care specialists and insurance providers to determine the most cost-effective yet efficient treatment strategies. This collaborative effort can lead to more accessible care for individuals in need, ensuring they receive the treatments that are indispensable to their health and healing.
To cap off, it's clear that for individuals with diabetes, particularly those in the Murray, UT area, there is an undeniable connection between diligent diabetes management and the reduction of chronic wound complications. By managing blood sugar levels, engaging in regular foot inspections and personalized care, and utilizing advanced wound care techniques, individuals with diabetes can greatly improve their outcomes.
It's crucial to embrace a proactive approach to health, seek knowledgeable partners in wound care, and leverage community resources designed to support and educate. The commitment to continuous care and the aspiration for an enhanced quality of life remain at the forefront for healthcare providers and those affected by chronic wounds.
Living with diabetes is an ongoing journey with thoughtful management and the help of a supportive medical community, the risks associated with diabetic wounds can be markedly diminished. As we strive for better health outcomes, let's champion the cause of holistic care, effective communication, and partnerships that empower individuals to lead healthier, more fulfilling lives.
Take charge of your health today by understanding the critical connection between diabetes and wound healing.
Reach out for expert advice and personalized care plans that work for you.